The study of the microbiota has disproportionately surprised the scientific sector, to such an extent that it may be one of the keys to treating obesity and other associated illnesses
How can some creatures that live inside us, are alive, breathe, feed and produce substances, control our body’s health in ways we haven’t even begun to imagine?
It is a question that we still cannot answer.
Index
Microbiota, bacteria that inhabit us
The microbiota is larger than us in number of cells and genes, with up to 3 trillion cells, 1000 different species and 3 million genes. We poor human beings have 10 times fewer cells and our genes are approximately 23,000.
We are small next to our bugs
In addition, they have been on this planet much longer than us. If we divide the evolution of planet earth into a month of 30 days (one day would be equivalent to 150M years), the first prokaryotic beings would appear on day +6, while the first eukaryotes would make their appearance on day +13. It isn’t until the last minutes of the last hour of the day +30 (last day) when the humans (us) make their appearance.
Beings that ferment
The bacteria that make up our microbiota feed on what we send them
Fermentation of dietary fibre
In this regard, the discovery of Short Chain Fatty Acids or SCFAs was revolutionary. These are small, short-chain fatty acids that are produced by the microbiota when fermenting dietary fibre and that have been shown to be beneficial at the metabolic level through different pathways.
It is postulated that the microbiota is largely responsible for the success of dietary fibre in practically any epidemiological or intervention study in which its role is evaluated. Why?
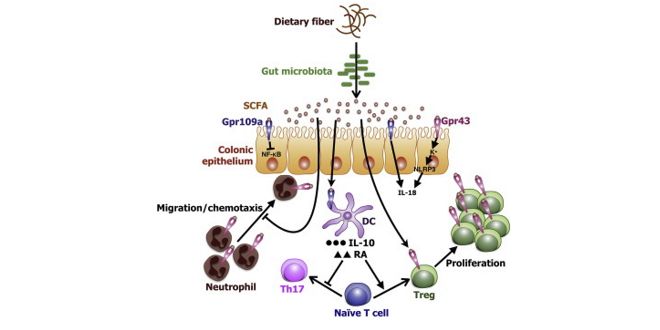
Because it is responsible for converting some of that dietary fiber into “good stuff” for us
Proteolytic fermentation
There is another type of fermentation, proteolytic fermentation, which takes place in the distal colon when the availability of MACs is low there, and which transforms proteins and amino acids into substances that do not seem to benefit the host as much.
They are indoles, phenolic compounds, branched chain fatty acids (BCFAs) or amines such as TMA (trimethylamine), cadaverine or putrescine.
Western Diet Problem
Evidence Linking Obesity to Intestinal Dysbiosis
How can the microbiota influence a person to maintain and develop Obesity:
Improvement of insulin resistance
A very fashionable nutritional strategy in recent years consists precisely in increasing the availability of accessible carbohydrates to the microbiota in the distal colon to increase the production of acetate, propionate and butyrate (the SCFAs that I spoke about before), in addition to of succinate, which seem to have shown a decrease in insulin resistance associated with obesity, improvement in weight loss, feeling of satiety and homeostasis of glucose and lipids (1 )(2)(3).
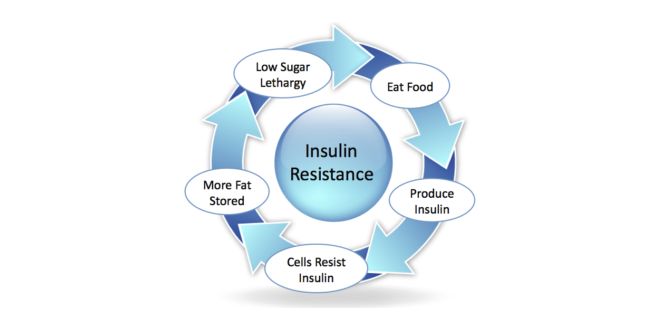
Insulin resistance cycle
Appetite suppressant effect
A study in mice demonstrated how SFCAs have a suppressive effect on appetite and energy intake through mechanisms that regulate the gut-brain axis. The acetate produced in the colon by the microbiota can pass the blood-brain barrier and reach the hypothalamus, producing an increase in the production of lactate and GABA, which in these animals considerably decreased appetite and energy intake ( 4).

A healthy microbiota produces more satiety
Increase energy expenditure
SCFAs are also in the spotlight because they plausibly have the potential to increase host energy expenditure
In obese mice, the oral administration of butyrate produced a decrease in body weight through an increase in energy expenditure and lipid oxidation (5). This effect was associated with upregulation of the expression of thermogenesis-related genes such as PGC1a or UCP1 in brown adipose tissue. But we are not only talking about animals, in humans we have in vivo data.
Body weight
Virtually all epidemiological and intervention studies in humans show an inverse relationship between dietary fibre and body weight, as discussed above (7).
Fibre supplementation
Transplanting the Microbiota
One of the most fascinating investigations in the microbiota studied what would happen if we transplanted the microbiota of two human twins, one obese and the other thin, into germ-free rats (that is, without any germs inside them).
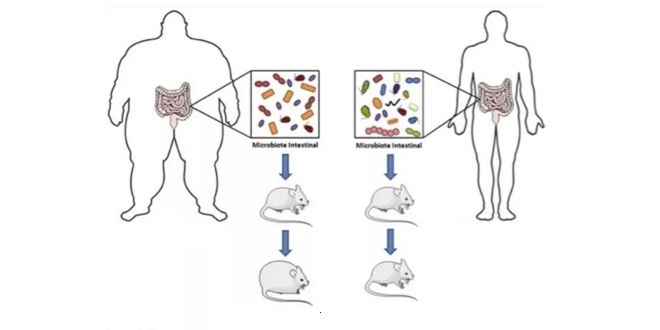
What happened was as expected, the microbiota of the obese twin transplanted into germ-free lean mice, transformed those lean mice into obese mice, establishing something very important: CAUSALITY (9)
In addition, the mice with the transplanted microbiota of the obese showed:
- Greater adiposity,
- Cecal concentrations (in the cecum, a part of the colon) of SCFAs, and
- Higher concentrations of monosaccharides and disaccharides after fiber intake.
In addition, they showed higher expression of genes involved in the expression of several aromatic amino acids and higher levels of BCAAs (plasma branched chain amino acids) in plasma than mice with the microbiota of the lean.
Conclusions
So far today’s evidence. New and more forceful will continue to appear and open our mouths
For now:
- Increase your intake of dietary fiber,
- Take care of your microbiota from harmful agents that are very present in our diet and lifestyle, and above all,
- Start soon.
See you in the next post. Keep empowering!
Bibliographical Sources
- Zhao L, Zhang F, Ding X, Wu G, Lam YY, Wang X, et al. Gut bacteria selectively promoted by dietary fibers alleviate type 2 diabetes. Science (80- ). 2018;
- Kovatcheva-Datchary P, Nilsson A, Akrami R, Lee YS, De Vadder F, Arora T, et al. Dietary Fiber-Induced Improvement in Glucose Metabolism Is Associated with Increased Abundance of Prevotella. Cell Metab. 2015;
- De Vadder F, Kovatcheva-Datchary P, Goncalves D, Vinera J, Zitoun C, Duchampt A, et al. Microbiota-generated metabolites promote metabolic benefits via gut-brain neural circuits. Cell. 2014;
- Frost G, Sleeth ML, Sahuri-Arisoylu M, Lizarbe B, Cerdan S, Brody L, et al. The short-chain fatty acid acetate reduces appetite via a central homeostatic mechanism. Nat Commun. 2014;
- Gao Z, Yin J, Zhang J, Ward RE, Martin RJ, Lefevre M, et al. Butyrate improves insulin sensitivity and increases energy expenditure in mice. Diabetes. 2009;
- Canfora EE, Van Der Beek CM, Jocken JWE, Goossens GH, Holst JJ, Olde Damink SWM, et al. Colonic infusions of short-chain fatty acid mixtures promote energy metabolism in overweight/obese men: A randomized crossover trial. Sci Rep. 2017;
- Menni C, Jackson MA, Pallister T, Steves CJ, Spector TD, Valdes AM. Gut microbiome diversity and high-fibre intake are related to lower long-term weight gain. Int J Obes. 2017;
- Cani PD, Joly E, Horsmans Y, Delzenne NM. Oligofructose promotes satiety in healthy human: A pilot study. Eur J Clin Nutr. 2006;
- Ridaura VK, Faith JJ, Rey FE, Cheng J, Duncan AE, Kau AL, et al. Gut microbiota from twins discordant for obesity modulate metabolism in mice. Science (80- ). 2013;
- Newgard CB, An J, Bain JR, Muehlbauer MJ, Stevens RD, Lien LF, et al. A Branched-Chain Amino Acid-Related Metabolic Signature that Differentiates Obese and Lean Humans and Contributes to Insulin Resistance. Cell Metab. 2009;
Related Posts
- What is SIBO (Bacterial Overgrowth)?
- How can the intestinal flora be improved?
- What are Prebiotics?
- What are Probiotics?





 Fitness, Nutrition, Health and Sports Blog In the HSNstore Blog you will find tips about Fitness, sport in general, nutrition, and health – HSNstore.com
Fitness, Nutrition, Health and Sports Blog In the HSNstore Blog you will find tips about Fitness, sport in general, nutrition, and health – HSNstore.com